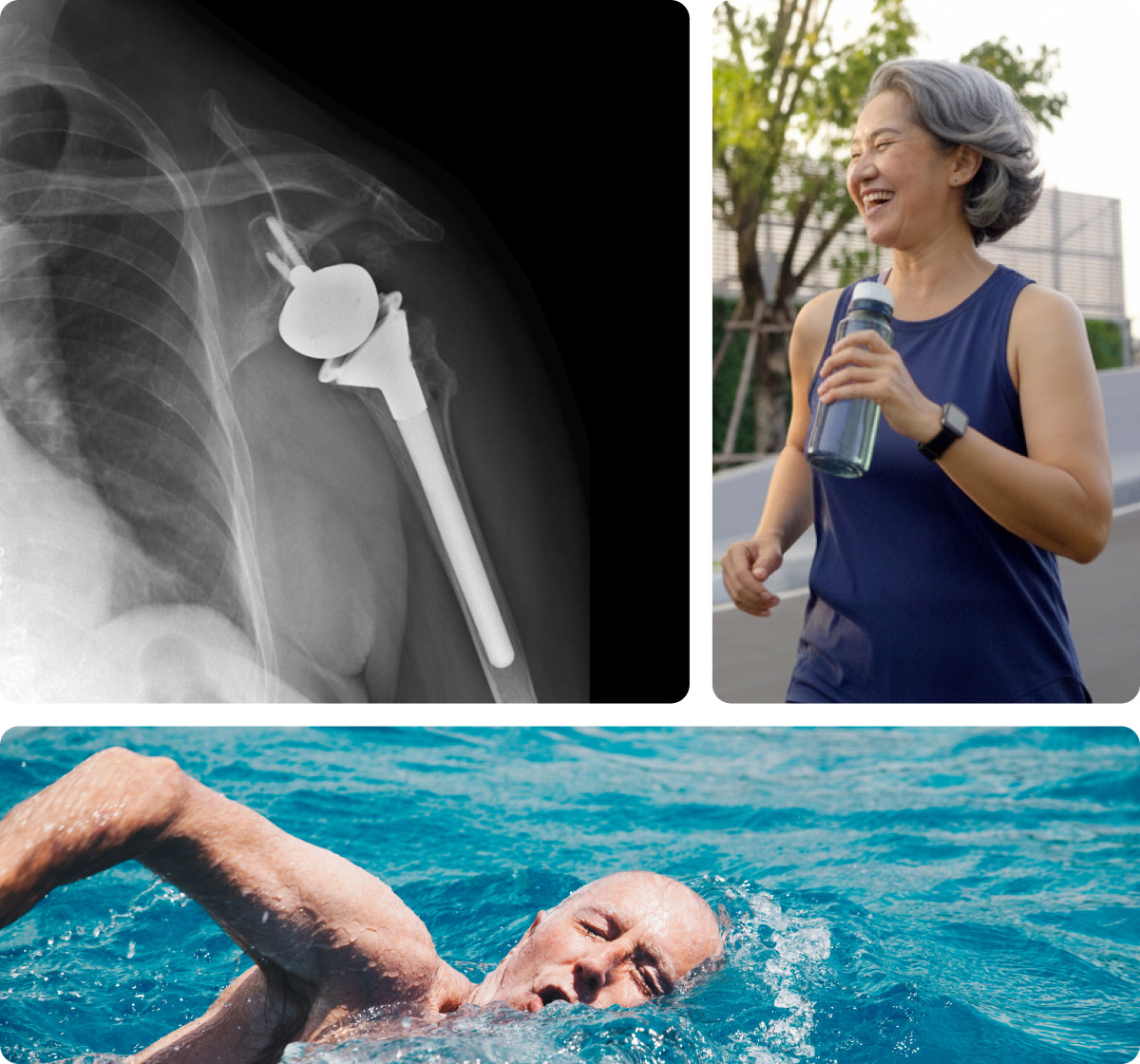
During total shoulder replacement, the damaged portions of the joint are removed and replaced with prosthetic components designed to restore smooth movement. The surgeon removes the worn head of the humerus and prepares the socket of the shoulder blade to properly position the implants.
A metal component is attached to the upper arm bone to form the new ball, while a durable plastic component is placed in the shoulder blade to create the socket. These implants may be secured with bone cement or designed to allow bone to grow into them for long-term stability.
By replacing the damaged joint surfaces, this procedure can significantly reduce pain and improve shoulder mobility, allowing patients to return to daily activities with greater comfort.
When We Would Recommend This Treatment
Total shoulder replacement is recommended when joint damage causes persistent pain and limited function that does not improve with conservative care such as physical therapy, medications, injections, or activity modification.
The most common cause is osteoarthritis, where cartilage gradually wears away, but other conditions such as rheumatoid arthritis, avascular necrosis, chronic rotator cuff damage, or fractures can also lead to joint deterioration.
When pain interferes with daily activities like lifting the arm, reaching overhead, dressing, or sleeping, and non-surgical treatments are no longer effective, shoulder replacement may be considered to restore function and relieve discomfort.
What to Expect
Before surgery, patients often experience significant shoulder pain, stiffness, and difficulty moving the arm. After total shoulder replacement, it is normal to have some soreness as the incision and surrounding tissues begin to heal. The arm is typically supported in a sling with an immobilizer for several weeks to help protect the joint during the early stages of recovery.
Physical therapy usually begins within the first few weeks following surgery to gradually restore range of motion and rebuild shoulder strength. Rehabilitation plays an important role in helping patients regain comfortable movement and improve overall shoulder function. Recovery timelines vary depending on the individual and the condition of the joint prior to surgery, but many patients experience meaningful pain relief and improved mobility over the course of several months as healing progresses.
Our Top-Rated Shoulder Providers
Three Common Conditions
Shoulder Osteoarthritis
Degeneration of cartilage leads to pain, stiffness, and reduced motion, and joint replacement can restore function when conservative treatments are no longer effective.
Rotator Cuff Tear
Degeneration of cartilage leads to pain, stiffness, and reduced motion, and joint replacement can restore function when conservative treatments are no longer effective.
Avascular Necrosis
Severe rotator cuff damage can lead to joint instability and degeneration, often treated with reverse shoulder replacement to restore arm function.
Frequently Asked Questions
Why might someone need a total shoulder replacement?
Total shoulder replacement is recommended when severe joint damage causes persistent pain, stiffness, and loss of function that does not improve with non-surgical treatment. Conditions such as osteoarthritis, inflammatory arthritis, fractures, or avascular necrosis can damage the joint surfaces, making everyday activities difficult. Replacing the joint can relieve pain and restore movement.
What types of shoulder replacement are available?
There are three main surgical options:
An anatomic shoulder replacement recreates the natural shape of the joint by replacing both the ball and socket. This option requires an intact rotator cuff and offers the most normal movement. A reverse replacement switches the positions of the ball and socket and relies on the deltoid muscle instead of the rotator cuff, making it ideal for patients with massive cuff tears. A partial replacement, or hemiarthroplasty, replaces only the ball when the socket is still healthy.
The choice of implant depends on the underlying condition and the quality of the soft tissues. Surgeons assess imaging and intraoperative findings to select the appropriate technique.
How should I prepare for shoulder replacement surgery?
Preparation begins with a thorough medical evaluation. The surgeon may order blood tests, an electrocardiogram, and imaging studies. It’s important to discuss current medications, including blood thinners and supplements. It may be recommended to stop certain medications before surgery to reduce bleeding risk. Smoking cessation and optimizing other health conditions, such as diabetes, can lower the risk of complications. Before the procedure, the patient receives instructions on fasting and what to expect at the hospital. Arrange for a ride home and assistance during the initial recovery period. Preparing a comfortable recovery space at home with pillows and easy-to-reach items can make the first few weeks easier. Following preoperative instructions helps ensure a smooth surgery and recovery.
What happens during and after total shoulder replacement surgery?
The surgery is performed under general anesthesia, sometimes combined with a regional nerve block for pain control. The surgeon makes an incision over the front of the shoulder, removes the damaged bone and cartilage, and inserts the prosthetic components. Once the new joint is in place, the incision is closed, and a sling is applied. After surgery, the patient spends time in a recovery area, and pain is managed with a combination of prescription medications and NSAIDs. Most patients go home the same day or after an overnight stay. An immobilizer is worn for several weeks to protect the repair while tissues heal. Physical therapy starts within a few weeks, focusing first on restoring motion and later on strengthening. Recovery is gradual, and improvement continues for several months.